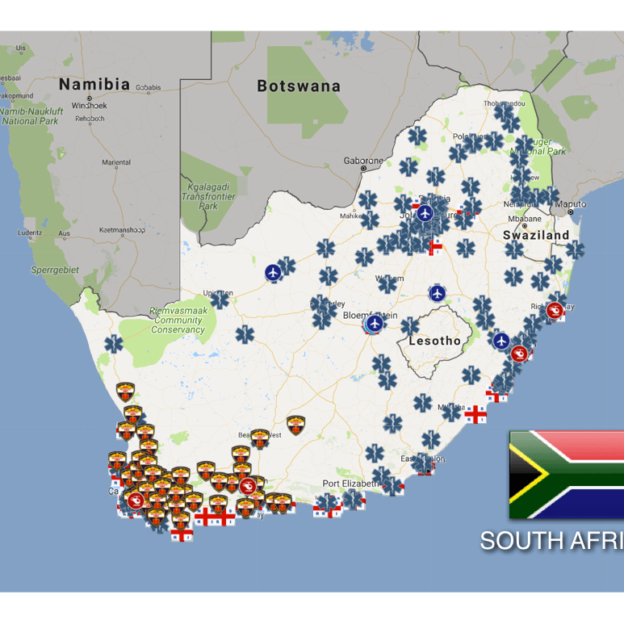
AT-A-GLANCE
TO CALL AN AMBULANCE IN SOUTH AFRICA DIAL 10177, or 112 (from mobile phones)
- In past 15 years, South African EMS has moved from isolated fire departments to sophisticated systems of ground and air response
- Coverage, resources and training vary from highest to lowest standards to none at all
- EMS personnel in South Africa experience a remarkable spectrum of clinical exposure
- Recently established specialty in emergency medicine should lead to greater political support and higher quality
HOW CAN I CALL AN AMBULANCE IN SOUTH AFRICA?
The toll-free number for emergency services in South Africa is 10177.
You can also call 112 from any cellphone.
You will then reach a call centre and they will route you to the closest emergency service. It’s also a good idea to familiarise yourself with the number of the ambulance service (either public or private) in your area and make sure you keep it handy – close to the phone or programmed into your cellphone.
No. It’s good to know the numbers of private ambulances as well.
South African response has high levels of disparity in coverage.
PRIVATE GROUND AMBULANCE SERVICES IN SOUTH AFRICA
EASTERN CAPE
- Adelaide
- Alderson Ambulance Service: +27 86 022 3366
- Aliwal North
- Gardmed Ambulance Service: 041 373 6777
- Butterworth
- Alderson Ambulance Service: +27 86 022 3366
- East London
- Alderson Ambulance Service: +27 43 726 2225
- Dynamic Emergency Medical Services Cc: +27 43 726 2225
- Maponya 911 Rescue (Summerpride): +27 86 196-0960
- Elliot
- Alderson Ambulance Service: +27 86 022 3366
- Grahamstown
- Netcare 911: 082-911
- Humansdorp
- Private Care Ambulance Service: +27 42 291 0749
- Mdantsane
- Hi-Care Emrs: +27 43 761 4339
- Mthata
- Gardmed Ambulance Service: +27 82 325 2143
- Umtata Ambulance Services: +27 47 532 4174
- Port Alfred
- Gardmed Ambulance Service: +27 82 759 2134
- Port Elizabeth
- Eastern Cape Medical Response: +27 41 365 7088
- Gardmed Ambulance Service: +27 41 373 6777
- Relay EMS: +27 861 061 061
- Trauma Net: +27 41 466 7342
- Queenstown
- Alderson Ambulance Service: +27 86 022 3366
- Uitenhage
- Relay EMS: +27 861 061 061
FREE STATE
- Bethlehem
- ER24: 084-124
- Bloemfontein
- ER24: 084-124
- Maponya 911 Rescue: (+27) 86 196 0960
- Netcare 911: 082-911
- Maselspoort
- Netcare 911: 082-911
- Parys
- Parys Medix: +27 83 559 0674
- Sasolburg
- Vaal Emergency Care: +27 16 976 7887
- Weklom
- ER24: 084-124
GUATENG
- Benoni
- Maponya 911 Rescue: +27 86 196 0960
- Brakpan
- AlertSA Ambulance Services: +27 72 838 8949
- Centurion
- Critical Life Assist: +27 60 911 0911
- MedAssist: +27 83 409 3694
- Rescue 786 Ambulance:+27 12 384 2336
- Gardenvale AH
- Baneshu EMS: +27 79 587 2474
- Germiston
- Emergency Medical Response Service (EMRS): +27 11 023 0911
- Johannesburg
- Amalgam – Rescue 786 Ambulance Services: +27 83 900 0786
- Contatia Kloof – Maponya 911 Rescue: +27 86 196 0960
- Diepkloof – Life Star 911 EMS Pty Ltd: +27 73 724 4486
- Mondeor – ER24: 084-124
- Orange Grove – Hatzolah Medical Rescue: +27 860 100 101
- Parkhurst – Destination Medicine Medical Rescue: +27 86 111 1138
- Randburg – High Tech Medical CC: +27 13 752 4470
- Sandton
- Destination Medicine: +27 78 327 3957
- Emer-G-Med (Pty) Ltd: +27 86 100 7911
- ER24: 084-124
- Medi Response Holdings (PTY) LTD: +27 11 713 2000
- National Emergency Medical Services: +27 86 100 6367
- SLA Paramedic Services: (+27) 11 465 4886
- Strijdom – Quick Response Service: +27 81 277 7777
- Johannesburg South
- Buthelezi EMS: +27 11 941 1555
- High Care EMS (Pty) Ltd: +27 86 100 0266
- Maponya 911 Rescue: +27 86 196-0960
- Med Help Emergency Services (Pty) Ltd: +27 61 399 0991
- Resqcare: +27 84 508 9111
- Supreme Care EMS: +27 11 432 5195
- Johannesburg West
- ER24: 084-124
- Krugersdorp
- Life Star 911 Ems Pty Ltd (Ambulance Services): +27 81 414 6222
- Lenasia
- Promed Ambulance Services: +27 73 776 6333
- Pulsate Emergency Medical Service: +27 82 714 2446
- Saaberie Christy Ambulance Services: +27 11 854 4618
- Midrand
- Carewell Ambulances: +27 11 039 5089
- Pretoria
- Annlin – Advanced Paramedic Assist +27 12 800 4205/ 12 800 2647
- East Lynne
- Advanced Paramedic Assist (APA): +27 12 800 4205/ 12 800 2647
- Maponya 911 Rescue: +27 86 196 0960
- Equestria – LifeMed Ambulance Service: 086 1086 911
- Lotus Gardens – Maponya 911 Rescue: +27 86 196 0960
- Mamelodi – Advanced Paramedic Assist: (+27) 12-800-4205 / (+27) 12-800-2647
- Meyerspark –Advanced Paramedic Assist: (+27) 12-800-4205 / (+27) 12-800-2647
- Mtn View – Bestcare EMS: +27 82 402 1416
- Villiera – LifeMed Ambulance Service: 086 1086 911
- Wilgers – LifeMed Ambulance Service: 086 1086 911
- Roodeport
- Quick Response Service: +27 81 277 7777
- Vitalmed: +27 87 095 1312
- Soweto
- Maponya 911 Rescue: (+27)86 196 0960
- Springs
- Maponya 911 Rescue: (+27)86 196 0960
LIMPOPO
- Bela Bela
- LifeMed Ambulance Service: 086 1086 911
- Groblersdal
- LifeMed Ambulance Service: 086 1086 911
- Giyania
- Genesis Emergency Medical Management: (+27)15 812 1544
- Lephalale
- Critical Life Assist: +27 60 911 0911
- Mokopane
- Maponya 911 Rescue: +27 86 196 0960
- Phalaborwa
- Maponya 911 Rescue: +27 86 196 0960
- Polokwane
- Maponya 911 Rescue: +27 86 196 0960
- ER24: 084-124
- Matsobane Ambulance Services: +27 78 963 6382
- Protoscape 202 Private Ambulance Service: +27 15 291 3778
- South African Paramedic Services: (+27)86 122 5599
- Thabazimbi
- Critical Life Assist: +27 60 911 0911
- Thohoyandou
- Eagle’s 911 Ambulance Service: +27 84 561 9900 / +27 73 710 0702
- TEMS 911: +27 81 463 0343
- Tzaneen
- LifeMed Ambulance Service: 086 1086 911
- Maponya 911 Rescue: +27 86 196 0960
- Tzaneen Ambulance Services: +27 15 306 0666
MPUMALANGA
- Bushbuckridge
- Maponya 911 Rescue: +27 86 196 0960
- Komatiepoort
- LifeMed Ambulance Service: 086 1086 911
- Malelane
- LifeMed Ambulance Service: 086 1086 911
- Middleburg
- ER24: 084-124
- Nelspruit
- Hi Tech Medical Services: +27 13 752 4470
- LifeMed Ambulance Service: 086 1086 911
- Piet Retief
- Piet Retief Private Ambulance Service: +27 17 826 3868
- Springs
- Grootvlei Nooddiens: +27 17 779 0234
- Standerton
- Trauma Sorg Acc: +27 82 700 3434
- White River
- Maponya 911 Rescue: +27 86 196 0960
- Witbank
- ER24: 084-124
NORTHERN CAPE
- Barkly West
- Netcare 911: 082-911
- Hartswater
- Netcare 911: 082-911
- Kathu
- Netcare 911: 082-911
- Kimberley
- Netcare 911: 082-911
- Kuruman
- Netcare 911: 082-911
- Ritchie
- Netcare 911: 082-911
- Springbok
- South African Paramedic Services: (+27)86 122 5599
- Upington
- SMS Rescue: +27 83 366 3888
KWAZULU NATAL
- Amanzimtoti
- Sisanda Medical Services: +27 81 247 6042
- Dolphin Coast
- IPSS Medical Rescue: +27 82 391 1911
- Durban
- Afromed Medical Services: +27 73 333 6656
- Isiqalo Life Rescue: +27 74 373 7283
- Rescue Care: +27 86 073 7911
- Citimed Ambulance: +27 80 033 3911
- Durban North
- Crisis Medics (Pty) Ltd.: +27 86 112 7474
- Empangeni
- Mounties Ambulance & Emergency Services: +27 86 124 7911
- Xtreme Medix: (+27) 83 389 5911
- Esikhawini H
- Xtreme Medix: (+27) 83 389 5911
- Estcourt
- AEMS: +27 36 352 2703
- Uthumed Ambulance Services: +27 36 352 1392
- Hillcrest
- Kwazulu Private Ambulance: +27 860 247 911
- Howick
- Berg Protection Services: +27 86 100 0098
- Kokstad
- Med-Evac CC: +27 82 940 1590
- Ladismith
- Sharaj Ambulance: +27 36 637 7933
- Mandini
- Xtreme Medix: +27 83 389 5911
- Manguzi
- Miles Medical Service: +27 81 771 1440
- Margate
- Kwazulu Private Ambulance: +27 76 435 7911
- Med-Evac CC: +27 82 940 1590
- Revival Med Rescue Specialists: +27 76 435 7911
- Mtubatuba
- Xtreme Medix: +27 83 389 5911
- Park Rynie
- South African Paramedic Services: +27 86 122 5599
- Umdoni Ambulance Service: +27 84 786 7911
- Phoenix
- Crisis Medical (Pty) Ltd: +27 86 112 7474
- Maponya 911 Rescue: +27 86 196 0960
- Pietermaritzburg
- KwaZulu Private Ambulance: +27 86 024 7911
- Maponya 911 Rescue: +27 86 196 0960
- Umhlanga
- Crisis Medical (Pty) Ltd: +27 86 112 7474
- Umlazi
- Maponya 911 Rescue: +27 86 196 0960
- Umtentweni
- Med-Evac CC: +27 82 940 1590
- Verulam
- Reaction Unit South Africa: +27 86 123 4333
- Vryheid
- KwaZulu Private Ambulance: +27 34 983 2162
NORTH WEST
- Carletonville
- ER24: 084-124
- Klerksdorp
- DKJ Ambulance Service: +27 72 826 4499
- Quickcare 24/7: +27 86 123 1233
- Intensive Medical Response (IMR) Paramedical Services: +27 18 468 5561
- Lichtenburg
- Golden Eye Medical Rescue: +27 18 632 4637
- Potchefstroom
- ER24: 084-124
- Rustenburg
- Trauma Rescue Ambulance Service: +27 86 178 9911
- Vryburg
- Gerijo Private Ambulance Service: +27 83 292 9111
- Wolmaranstad
- TAC-Pulse Emergency Response Services (PTY) Ltd.: +27 86 166 6911
- Zeerust
- Platinum Emergency Care Ambulance: +27 84 954 0818
WESTERN CAPE
- Beaufort West
- South African Paramedic Services: +27 86 122 5599
- Cape Town
- Atholone – Cape Medics: +27 21 697 4782
- Belville – ER24: 084-124
- Blaauwberg –Netcare 911: 082-911
- Brackenfell – Netcare 911: 082-911
- Brackenfell – ER24: 084-124
- Camps Bay – Community Medics: (+27) 83 379 9247
- Centre – Ezra Medical: (+27) 21 464 6766
- Centre – Netcare 911: 082-911
- Edgemead – Resq Medix: +27 74 173 7283
- Fish Hoek – Cape Medical Response: +27 21 782 0606
- Gardens – ER24: 084-124
- Gatesville – Melomed Gatesville: +27 21 637 8100
- Goodwood – Netcare 911: 082-911
- Kenilworth – Netcare 911: 082-911
- Kraaifontein – LC Medical: +27 82 319 1277
- Kuils River – Med-Life Ambulance: +27 44 533 6444
- Kuils River – Netcare 911: 082-911
- Kuils River – Taurus Medical: +27 82 710 9704
- Mansfied – GBMED-Rescue: +27 76 185 5351
- Milnerton – Medics In Motion: +27 21 551 3386
- Milnerton – ER24: 084-124
- Montaque – South African Paramedic Services: +27 86 122 5599
- Mowbray – South African Paramedic Services: +27 86 122 5599
- N1 City – Netcare 911: 082-911
- Parow – Tygerberg Emergency & Support Services (TYGESS): +27 21 952 8818
- Pinelands – Life Vincent Pallotti Hospital: +27-21-506 4176
- Plumstead – ER24: 084-124
- Plumstead – EMT-Emergency Medical Treatment CC: +27 86 038 6386
- Somerset West – Immediate Medical: +27 71 501 6007
- Somerset West – ER24: 084-124
- Strand – Emergency Medical Operations (EMO): +27 21 853 5978
- Strand – Immediate Medical: +27 71 501 6007
- Strand – Netcare 911: 082-911
- Table View – Community Medics: +27 83 379 9247
- Wetton – Wetton Emergency & Training Centre: Office; +27 21 761 6706
- Fishershaven
- EMR: Emergency Medical Rescue: +27 82 468 9844
- Gansbaai
- Overstrand Medical Response: +27 78 699 6995
- George
- Eden911: (+27)60 891 1911
- ER24: 084-124
- Netcare 911: 082-911
- Klawer
- South African Paramedic Services: +27 86 122 5599
- Knysna
- ER24: 084-124
- Langebaan
- Atlantic Medical Response: +27 22 772 2377
- Montagu
- Sozo Medical Rescue: +27 23 614 2628
- Mossel Bay
- ER24: 084-124
- Med-Life Ambulance: (+27) 44 533 6444
- Oudtshoorn
- Ambu 911: +27-44-272-2526
- Resq Pro: +27-73-433-5789
- Paarl
- ER24: 084-124
- Plettenberg Bay
- Med-Life Ambulance: (+27) 44 533 6444
- Stellenbosch
- ER24 (Corporate Head Office): +27 21 809 6500
- Worcester
- ER24: 084-124
AIR AMBULANCE SERVICES IN SOUTH AFRICA
Training varies according population and socio-economic levels:
- Public Sector – Insufficient personnel and poorly maintained vehicles and equipment due to financial restraints
- Private Sector – Growing competence to provide sophisticated pre-hospital care and exceptional clinical expertise
TRAINING LEVELS
Basic Ambulance Assistant (BAA):
- Min 1mo trainingCPR/AED
- First Aid
- Basic Vehicle Extrication
- Packaging Techniques
- Simple Trauma Mgmt
- O2, Entonox, Oral Glucose and Activated Charcoal
- Recommended industry standards: minimum BAA personnel on every EMS vehicle
Ambulance Emergency Assistant (AEA):
- Experience + 3-4mos. Training
- Neb Rx for Asthma
- IV and Fluids
- IV glucose
- Aspirin
- Man. Defib
Critical Care Assistant (CAA):
- Similar to US Paramedic
- Experience + 9-12mos. full-time training
- Extensive emergency medical protocols designed along lines of:
- PALS
- ACLS
- ATLS
- Advanced Airway Mgmt
- Synchronized Cardioversion
- 27 different meds
- Benzodiazepines
- IV analgesics
- Emergency Cardiac meds
National Diploma in Emergency Medical Care:
- Post-Graduate study
- Top level of prehospital Emergency care practitioner
- Dedicated 3yr full-time training programs at specificpost-graduate technical colleges
- In-depth Anatomy/Physiology
- Wide range of related disciplines
- Rescue
- Communications
- “They may, in fact, be amongst the best trained paramedics in the world” (Macfarlane, 147)
- Thoroughness and Extent of Training
- Significant on-road experience
- High quality of advanced medical instruction
- May extend academic training by completing 4thyr and graduating with a Bachelor of Technology degree
The vehicles used by EMS in South Africa can vary greatly across a broad range. They may be large or small, new or quite old, often driven by local economics. There is no specific current standard for ambulance design in South Africa. Some vehicles comply with either the European standard CEN 1789 or the US standard, KKK-1822, but many meet neither standard. There are even examples of motorcycles with stretcher-carrying sidecars.[17] There is currently a major initiative underway by the government of South Africa to replace much of the aging fleet with new high standard emergency ambulances. Plans call for the replacement of approximately 450 ambulances by 2010.[18]
Source: WIKIPEDIA
Helicopter EMS and other specialized rescue services are also available:
- Single national coordinating service
- Run under auspices of Air Mercy Service of the Red Cross
- 5 dedicated helicopters in the major metropolitan areasJohannesburg 24h twin-engine service was once busiest in world
- Private-operated fixed-wing air evacuation, both nationally and into sub-saharan AfricaHospitals frequently receive poly-trauma/complicated medical cases from entire Southern African region
“The amount will depend on how much you earn and on how many dependants you have, according to the hospital rating scale.
At the low end of the scale – that is, if you are unemployed – you will be expected to pay R39 as an outpatient. This will cover your consultation, medication and possible blood or other tests. A pensioner will pay only R13 for the same service. If you are unemployed and need to be admitted, you will pay R194 for up to 30 days.
The maximum a state hospital will charge, if you’re at the top end of the income scale, is R55 for a consultation. However, you will be charged additional amounts for medication and tests. For a stay in hospital, a top-end patient (including those on medical aid) will pay R484.90 per day, excluding medicine and theatre costs.
The government is trying to guide patients away from hospitals to its public clinics and community health care centres – where free primary health care services are available. However, patients on medical aids will be charged.
Specialized treatment and care is available at state hospitals, but waiting lists are often very long, depending on the problem or medical procedure needed. If you have medical aid cover it may be easier to go to a private hospital.”
Source: BrandSouthAfrica.com
“A service that has been designed specifically with international visitors in mind is the provision of travel assistance packages, costed at a daily rate, which include emergency assistance. These services include dedicated hotline numbers that can be called in case of an emergency and liaison with visitors’ travel insurers under such circumstances.
While they are not emergency service providers themselves, they use a network of such providers to respond to clients’ emergency needs.”
Source: country.southafrica.net
ADDITIONAL INFO
- 1910 – Act of Union: “The provision of ambulance services was designated to third tier government and thus fell under the local authority. Town clerks (in the interest of their ratepayers) combined firefighting and ambulance services into one service, thus presenting us with the Fire and Ambulance Service. With notable exceptions, and because of a lack of medical control and input the ambulance component of these services tended to lack support and thus problems were experienced with equipment, training and standards” (Dalbock, 1996)
- Late 1960s – Western Cape Ambulance Services are regionalized and a medical director assumes control of the services
- 1977 – A national law is passed making provision of ambulance services responsibility of the then four provincial administrations
- Basic ambulance services begin serving communities within local government boundaries, though services in many parts of country are still unavailable
- 1980s – Provinces work to develop comprehensive systems, including:
- Training academies (up to intermediate life support)
- Strategically located ambulance units
- Upgrades to communications systems
- Late 1980s – Services in four major urban centers have advanced care providers and are meeting established international standards, but “these islands of pre-hospital excellence, however, existed in a sea of mediocrity and large areas of the country had rudimentary if any, ambulance services with standards varying tremendously – depending on which service one inspected.” (Dolback, 119)
- This leads to fragmented services of varying norms and standards, and frustrates reciprocity among prehospital providers between provinces
- 1992 – Leads to the establishment of the Professional Board for Emergency Care Personnel who ultimately grant national recognition to ambulance practitioners by South African Medical and Dental Council.
- 1994 – New regulations are passed making it compulsory for all practitioners to register
- National curricula for emergency care established
- Great disparity of services available between provinces
- All have problems with use of services for mild injuries and illnesses
- Resulting drain on resources
- Public education, better public transport and availability of more basic patient transport vehicles required
- All have problems with use of services for mild injuries and illnesses
Lead Agency
Emergency ambulance service is provided by each South African province. The system of government-operated ambulances is generally referred to as ‘Metro’
Source: WIKIPEDIA
Government Oversight
- March 2004 – Emergency Medicine officially established/recognized as separate medical specialty
- Gov’t Hospitals
- Modelled on former UK “Casualty Departments”
- Significant Patient overload
- Large number of ambulatory, non-emergent Patients
- Many are primary health care Patients that have bypassed local clinics
- Patients s can be impatient, aggressive and can resent more serious cases being attended before them
- Private Hospitals
- Well-developed and extensive private sector, many of which have EDs
- Many EDs are essentially general practices
- Non-regular presentation of “true emergencies”
- Well-developed and extensive private sector, many of which have EDs
Funding
- Services funded by individual provinces from funds allocated by national gov’t; EMS Care free of charge to all earning below certain threshold
Dispatch
- Call centers have varied capabilities with more sophisticated using software programs for triage and appropriate vehicle dispatch
- No formal EMD training courses yet implemented for most call center personnel
- Response Time Goals
- Urban – 15mins
- Rural – 40 mins
- Greater Johannesburg only reported district to achieve these goals “semi-regularly”
- Dalbock C: “A history of ambulance practitioners and services in South Africa.” SA Family Practice1996;17:118-121
- Govender K, Grainger L, Naidoo R. “Developing retention and return strategies for South African advanced life support paramedics: A qualitative study.” Afr J Emerg Med. 2013 Feb 21;:1–8.
- Govender K, Grainger L, Naidoo R, MacDonald R. “The pending loss of advanced life support paramedics in South Africa.” Afr J Emerg Med. 2012 Jun 1;2(2):59–66.
- Hackland S, Stein C. “Factors influencing the departure of South African advanced life support paramedics from pre-hospital operational practice.” Afr J Emerg Med. 2011 Jun 1;1(2):62–8.
- MacFarlane C, van Loggerenberg C, Kloeck W: “International EMS Systems: South Africa – Past, Present and Future.” Resuscitation2005;65:145-8.
- Newton PR, Naidoo R, Brysiewicz P. “The appropriateness of emergency medical service responses in the eThekwini district of KwaZulu-Natal, South Africa.” S Afr Med J. 2015 Sep 29;105(10):844–4.
- Stein C, Wallis L, Adetunji O. “Meeting national response time targets for priority 1 incidents in an urban emergency medical services system in South Africa: More ambulances won’t help.” S Afr Med J. 2015 Sep 29;105(10):840–5.
- Health Professions Council of South Africa
- Report: “Emergency Medical Services in the Eastern Cape” Treatment Action Campaign (TAC) (2015)
- Hearing Report: “Access to Emergency Medical Services in the Eastern Cape” South African Human Rights Commission (March 24 & 25 2015)
- Presentation: “Free State Emergency Medical Services – 2015 Strategic Plan”
SCOREBOARD
% of Seriously Injured Patients Transported by Ambulance in South Africa, 2013
[Source: 2013 Global Status Report on Road Safety, WHO]
ROAD TRAFFIC INJURY DEATHS
(PER 100,000 POPULATION)
[Source: 2015 Global Status Report on Road Safety, WHO]
REPORTED HOMICIDES
(PER 100,000 POPULATION)
[Source: 2014 Global Status Report on Violence Prevention, WHO-UNDP]
ASSAULTS AGAINST PARAMEDICS AND DRIVERS – 2016
Reported in Western Cape province last year.
[Secondary source: TheNation.ae]